Reframing Care

Reframing Care
For decades, healthcare systems have been optimized for the physician’s time and asset utilization at the expense of patient experience. Patients are funneled through hospital buildings, diagnostic imaging centers, and physician clinics like products on an assembly line. This care model is outdated.
Care delivery must be upgraded post-pandemic to optimize the healthcare workforce, starting with nurses, resulting in better patient experiences and improved outcomes. Human-Centered Health reframes care delivery in a holistic system of 3 patient care circles:
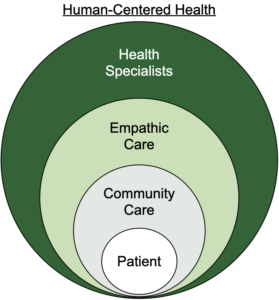
- Community Care: Family, friends, and community members who provide love, support, and assistance.
- Empathic Care: Nurses and other caregivers with compassionate listening skills and broad healthcare experience translate technical jargon and help navigate the healthcare journey.
- Health Specialists: Physicians and other caregivers with deep domain expertise and technical skills needed to execute healthcare procedures and services to deliver the patient’s care plan.
The patient sits at the center, surrounded by family and friends in their community care circle. Then, nurses and other empathic caregivers are empowered to listen to the patient and guide them through the healthcare journey. These caregivers help recognize potential complications and take appropriate action. Health Specialists, such as surgeons, deliver highly-specialized care but often do not have enough time to provide empathic care. Coordination of these three levels of care results in better patient experiences and improved health outcomes.
Elevate the Nurse
Traditional healthcare over-emphasizes the technical skills of Health Specialists. Our model corrects this imbalance by elevating nurses as the primary point of contact between the patient and the system as empathic caregivers. Nurses bring compassionate listening skills combined with broad healthcare experience, making them well-suited to advise the patient, thereby improving health outcomes and reducing costs.
During the hospital stay, patients are diagnosed, receive treatment, and then recover until they can be discharged. The patient often suffers pain and discomfort during their stay as a part of the treatment. Bedside staff help patients in their struggles but rarely get to celebrate their full recovery. Nurse burnout is partly caused by the constant stream of suffering patients combined with a lack of ability to witness their patient’s recovery and return to the joys of everyday life.
The empathic caregiver role extends beyond the patient’s discharge. New tools and processes free nurse capacity allowing them to build longer-term, meaningful relationships with their patients via calls and text messages. With this approach, patients experience greater continuity of care, and nurses earn additional compensation while seeing their patients through the entire healing process.
Best of all, these services are reimbursable under existing Medicare codes for Remote Patient Monitoring (RPM) and Chronic Care Management (CCM). By reframing care delivery to support patients at the three levels of community care, empathic care, and health specialists, Human-Centered Health optimizes the patient’s health and quality of life, creates new streams of revenue, and empowers bedside staff to help patients during acute care recovery and over their entire health journey.

